About Sun River Health
At Sun River Health, we believe that excellent health care should not be a privilege for a few, but a right for all.
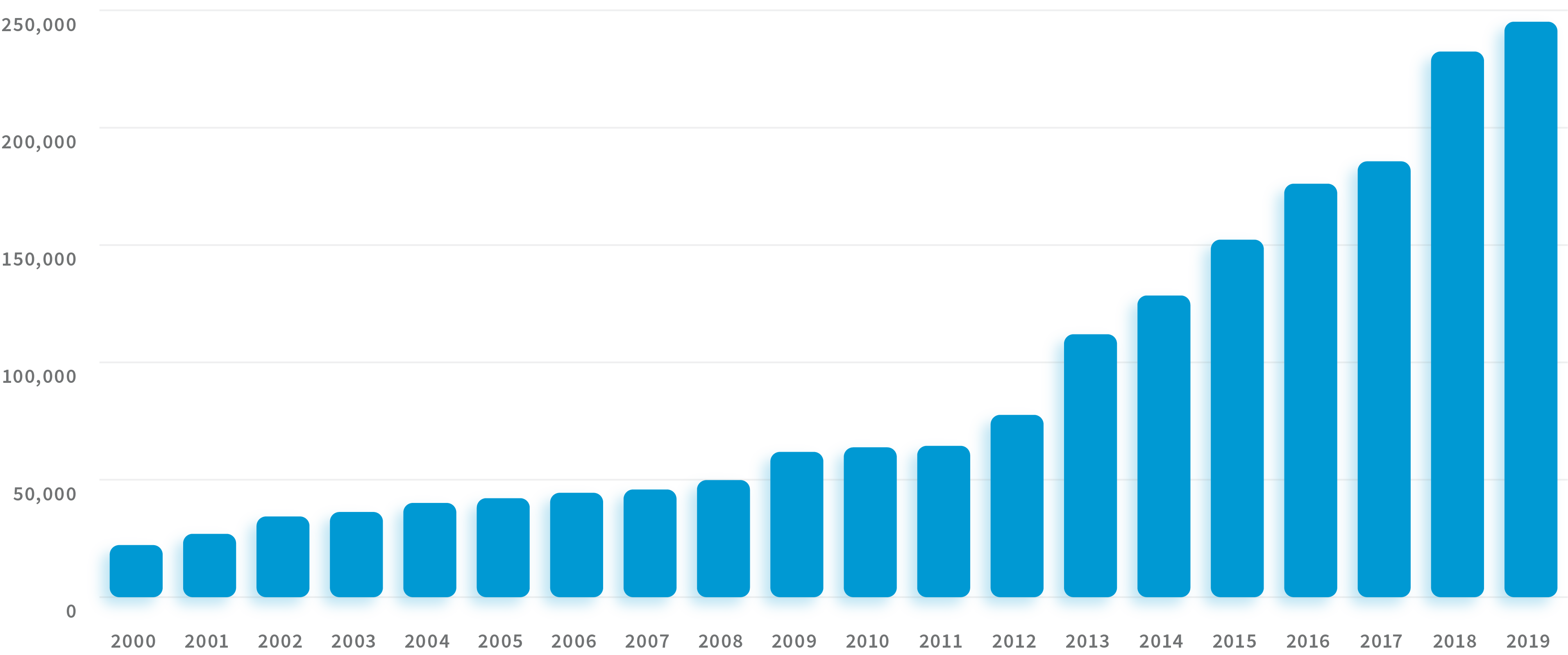
As of today, more than 250,000 patients count on Sun River Health to get the care they need and the respect they deserve. They can access 400+ providers in 48 health centers across the Hudson Valley, New York City, and Long Island.
Recognition & Awards

MISSION
To increase access to comprehensive primary and preventive health care and to improve the health status of our communities, especially for the underserved and vulnerable.
Accreditations | Year |
|---|---|
Primary and behavioral health care services by Joint Commission | 1998 |
Federally Qualified Health Center | |
FTCA Deemed OrganizationThis health center is a Health Center Program grantee under 42 U.S.C 254b, and a deemed Public Health Service employee under 42 U.S.C 233(g)-(n). Therefore, HRHCare is granted medical malpractice liability protection through the Federal Tort Claims Act (FTCA), and are considered Federal employees with the Federal government acting as their primary insurer. |
Recognition | |
|---|---|
National Committee on Quality Assurance (NCQA) Patient-Centered Medical Home | 2009 |
Selected by the National Centers for Disease Control (CDC) as one of the nine worksite wellness programs nationwide used to help other employers in designing and executing worksite wellness programs. | |
Planetree DesignationThe Planetree Designation represents the highest level of achievement in patient-centered care based on evidence and standards. HRHCare earned the Planetree Designation in 1996 and continues to honor Planetree evidence based standards. HRHCare remains the only Federally Qualified Health Center to achieve the Planetree Designation. |
Awards | |
|---|---|
The HIMSS Davies Community Health Organization Award of ExcellenceFor outstanding achievement in the implementation and value derived from the electronic health record to improved patient care and health outcomes. | |
U.S. Department of Health and Human Services Innovation in Prevention | 2006 |
New York State Patient Safety | 2006 |
Public Health Partnership Award from the Dutchess County Department of HealthMaternal-Infant Care Program 2000 | 2006 |
U.S. Department of Health and Human Services Models That Work Award for Sun River HealthMaternal-Infant Care Program (2000) |
Memberships | |
|---|---|
National Association of Community Health Centers | |
Community Healthcare Association of New York State |
“I liked the attention from the assistant, the nurse, the doctor, and the transport driver who picked us up and took us back. They took excellent initiative.”
— Emmanuel, Sun River Health The Hub patient
Quality care. Fair cost.
No one should ever go without health care. If you lack insurance or the ability to pay in full, Sun River Health is here for you.